- The DASH diet, the Nordic diet, and the Mediterranean diet are effective for lowering blood pressure in patients with hypertension.
- Bariatric surgery has been shown to both cause significant weight loss and to prevent the development of type 2 diabetes.
- The Weight Watchers, Jenny Craig, and Nutrisystem diets appear to enable significant weight loss in patients who adhere to the programs.
- For all the approaches – except for bariatric surgery – adherence is a significant issue affecting clinical efficacy.
A number of diets, as well as bariatric surgery, have been found in meta-analyses and randomized controlled trials (RCTs) to help patients lose weight, reduce blood pressure, and prevent the onset of type 2 diabetes mellitus (T2DM). This article examines the data supporting diets and surgery, and the evidence that they can benefit patients at risk of hypertension, obesity, and T2DM.
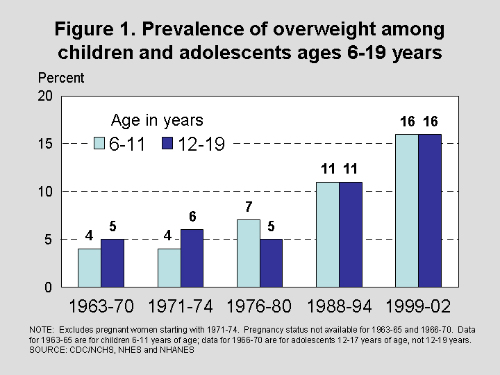
Diets
Advances in Nutrition
A systematic review and meta-analysis published recently in Advances in Nutrition (2016:15;7[1]:76-89), “Dietary Patterns and Blood Pressure in Adults: A Systematic Review and Meta-Analysis of Randomized Controlled Trials,” included 17 RCTs. The aim of this study was to assess the effect of dietary patterns on blood pressure in adults. The results show that the DASH diet, the Nordic diet, and the Mediterranean diet significantly lowered systolic blood pressure and diastolic blood pressure by 4.26 mmHg and 2.38 mm Hg, respectively.
These diets are rich in fruit, vegetables, whole grains, legumes, seeds, nuts, fish, and dairy and low in meat, sweets, and alcohol. “Lifestyle factors such as exercise and weight loss in combination with dietary changes may also reduce blood pressure” the authors noted.
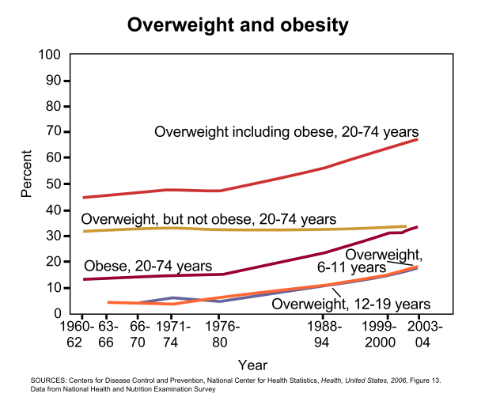
Annals of Internal Medicine
A systematic review published recently in Annals of Internal Medicine (2015;162:501-12), “Efficacy of commercial weight-loss programs: an updated systematic review,” examined 45 studies, including 39 RCTs.
The reviewers found that participants in the Weight Watchers program achieved ≥2.6% greater weight loss than those assigned to control/education. Participants in the Jenny Craig diet program were able to achieve ≥4.9% greater weight loss at 12 months compared with those who received education and counseling. Participants in the Nutrisystem program achieved ≥3.8% greater weight loss at 3 months versus controls who received education and counseling.
Participants in very-low-calorie programs such as Health Management Resources, Medifast, and Opifast were able to achieve ≥4.0% greater short-term weight loss compard whose who received counseling. However, the weight loss effect was diminished at >6 months. Patients who adopted the Atkins diet achieved 0.1% to 2.9% greater weight loss at 12 months compared with those who received counseling. Atkins patients frequently regained the lost weight at >12 months, according to a study published in Circulation: Cardiovascular Quality and Outcomes (2014 Nov;7(6):815-27). Results for the SlimFast diet were mixed.
“We found limited evidence to evaluate adherence or harms for all programs and weight outcomes for other commercial programs,” the reviewers noted. “Many trials were short (<12 months), had high attrition, and lacked blinding,” they noted.
“Clinicians could consider referring overweight or obese patients to Weight Watchers or Jenny Craig. Other popular programs, such as Nutrisystem, show promising weight-loss results; however, additional studies evaluating long-term outcomes are needed,” the authors concluded.
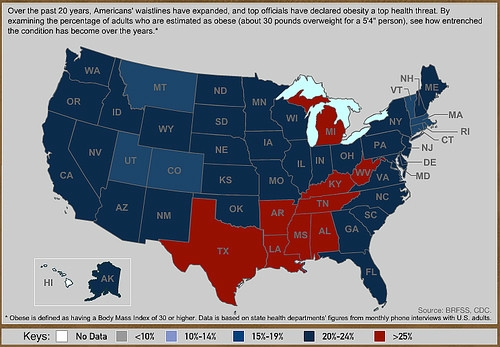
American Journal of Medicine
A report published recently in the American Journal of Medicine (2015 Dec 22. pii: S0002-9343(15)30027-9), “Systematic Review of the Mediterranean Diet for Long-Term Weight Loss,” described a review of RCTs examining the effect of the Mediterranean diet on weight loss and cardiovascular risk factor levels at ≥ 12 months. This analysis included 5 RCTs and 998 patients. The authors acknowledged that “the long-term health benefits of the Mediterranean diet are well established.”
However, this meta-analysis examined the effects of the Mediterranean diet on weight loss and cardiovascular risk factors after ≥12 months “Our findings suggest that the Mediterranean diet results in similar weight loss and cardiovascular risk factor level reduction as comparator diets in overweight or obese individuals trying to lose weight,” the authors concluded.
PLoS One
A study published in PLoS One, “Dietary Intervention for Overweight and Obese Adults: Comparison of Low-Carbohydrate and Low-Fat Diets. A Meta-Analysis” (2015:20;10:e0139817) reports that both low-fat (LoFAT) and low-carbohydrate diets (LoCHO), when adhered to strictly, result in significant weight loss. Of course, as any clinician knows, strict adherence is the greatest challenge for patients.
“This trial-level meta-analysis of randomized controlled trials comparing LoCHO diets with LoFAT diets in strictly adherent populations demonstrates that each diet was associated with significant weight loss and reduction in predicted risk of ASCVD [atherosclerotic cardiovascular disease] events.”
The researchers found a single advantage to the low-carbohydrate diet: The LoCHO diet was associated with modest but significantly greater improvements in weight loss and predicted ASCVD risk in studies from 8 weeks to 24 months in duration. “However,” they wrote, “LoCHO diet was associated with modest but significantly greater improvements in weight loss and predicted ASCVD risk in studies from 8 weeks to 24 months in duration. These results suggest that future evaluations of dietary guidelines should consider low carbohydrate diets as effective and safe intervention for weight management in the overweight and obese.”
Endocrine
A large meta-analysis was published in Endocrine (2014;47[1]:107-16). The analysis included 18 prospective studies with 20 cohorts in 4 world regions and more than 21,000 cases of incident diabetes.
The review, “Which diet for prevention of type 2 diabetes? A meta-analysis of prospective studies,” followed patients for approximately 10 years. The reviewers found that the Mediterranean and DASH diets significantly reduced the risk of developing T2DM (P=0.0487), but the evidence was limited to 2 studies. “The results of our study demonstrate that several healthy diets are equally and consistently associated with a 20% reduced risk of future type 2 diabetes,” the authors concluded.
British Journal of Nutrition
The DASH diet was originally constructed as a low-sodium diet designed to reduce hypertension. However, the diet has proven to be at least as effective for weight loss, and prevention of diabetes and heart disease as it for reducing blood pressure.
The study published in the British Journal of Nutrition (2014;11:28:1-15), “Effects of the Dietary Approach to Stop Hypertension (DASH) diet on cardiovascular risk factors: a systematic review and meta-analysis,” reported on a systematic review of RCTs designed to determine the effects of the diet on cardiovascular risk factors. The meta-analysis included 20 RCTs and 1917 participants.
The DASH diet was found to result in significant decreases in systolic blood pressure (P<0·001) and diastolic blood pressure (P<0·001). The diet also reduced the concentrations of total cholesterol (P<0·001), and LDL (P=0·03). “These changes predicted a reduction of approximately 13% in the 10-year Framingham risk score for cardiovascular disease (CVD).
“The DASH diet improved cardiovascular risk factors and appeared to have greater beneficial effects in subjects with an increased cardiometabolic risk. The DASH diet is an effective nutritional strategy to prevent CVD,” the reviewers concluded.
Nutrition
Results of systematic review published in Nutrition (2013;29[7-8]:939-47), “Effects of Dietary Approaches to Stop Hypertension (DASH) diet on some risk for developing type 2 diabetes: a systematic review and meta-analysis on controlled clinical trials,” found similarly positive results for the DASH diet. This meta-analysis included 20 RCTs and found that the DASH diet can significantly reduce fasting insulin concentration (P<0.001). Subgroup analysis showed that the DASH diet could significantly reduce fasting insulin levels when followed for >16 weeks (P<0.001).
“The DASH dietary pattern may lead to an improvement in insulin sensitivity independent of weight loss. The DASH diet may play an important role in glycemic control in long- term interventions,” the reviewers concluded.
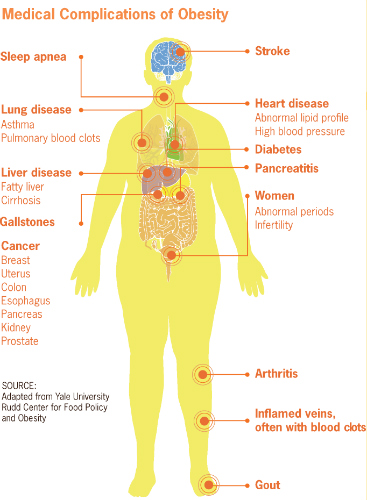
Bariatric Surgery
Philip Schauer, MD, of the Metabolic Institute at Cleveland Clinic has published results of 2 studies that show bariatric surgery to be a highly effective means of achieving enduring weight loss for patients who are overweight or obese. These study have also revealed a surprising finding: The weight loss often resulted in a reversal of type 2 diabetes in these patients. (See our video interview with Dr. Schauer here.)
The studies conducted by Dr. Schauer, et al, are as follows:
- “Bariatric surgery versus intensive medical therapy for diabetes--3-year outcomes.” (N Engl J Med. 2014;370(21):2002-13). The authors concluded that “Among obese patients with uncontrolled type 2 diabetes, 3 years of intensive medical therapy plus bariatric surgery resulted in glycemic control in significantly more patients than did medical therapy alone. Analyses of secondary end points, including body weight, use of glucose-lowering medications, and quality of life, also showed favorable results at 3 years in the surgical groups, as compared with the group receiving medical therapy alone.”
- In the paper called “Bariatric surgery versus intensive medical therapy in obese patients with diabetes,” (N Engl J Med. 2012;366:1567-76) Dr. Schauer and colleagues concluded that, “In obese patients with uncontrolled type 2 diabetes, 12 months of medical therapy plus bariatric surgery achieved glycemic control in significantly more patients than medical therapy alone.”
- In correspondence regarding the clinical trials they conducted, Dr. Schauer and colleagues wrote, “Given that the lifetime medical costs of treating type 2 diabetes and its complications are in the range of $124,000 to $130,000 (with an age at onset of 25 to 44 years), bariatric surgery—which has been shown to be cost-effective and possibly cost-saving—seems reasonable for patients whose condition is not well controlled with medical management alone.”
