- Implementation of drug monitoring programs was associated with reductions in opioid prescribing, opioid-related overdoses, and opioid-related overdose deaths.
- Prescription-drug monitoring programs, in effect in 49 of 50 states, were found to be effective in reducing opioid-related deaths.
- The programs were found to be cost effective and clinically effective.
- Clinicians expressed satisfaction with the programs in a majority of cases
Prescription-drug monitoring programs in a number of states have been shown to reduce opioid-related (Figure 1) deaths. The programs collect data from pharmacies on the prescribing of controlled substances, review and analyze the data, and report them to prescribers. As of 2014, 49 states had implemented drug-monitoring programs. And, according to the results of a study published recently in Health Affairs, the programs are effective in reducing a number of types of drug-related injury.
In the states that have such programs—all have them but Missouri—the data show that they improved clinicians’ confidence in opioid prescribing, identified and reduced doctor shopping, decreased overall opioid prescribing and treatment facility admissions, reduced diversion of, and improved clinicians’ ability to monitor opioid dependency treatment, according to the report in Health Affairs. Both clinicians and patients have generally be very satisfied with the results.
(Sources: Wikipedia/By Protein Data Bank (Protein Data Bank) CC BY-SA 3.0,
via Wikimedia Commons.)
Besides reducing the harm cause caused by opioids, the programs can also facilitate referrals to substance abuse treatment and help clinicians devise prevention strategies. “As the use of these programs becomes more common and consistent, their effect on decreasing the prescription opioid epidemic is likely to grow,” the authors wrote in Health Affairs.
The number of prescriptions for opioids has skyrocketed in the, 259 million prescriptions were written annually for opioid analgesics—more than one ‘script for every US adult, every year. As the number of prescriptions increased, so did complications from the drugs’ use and misuse, including neonatal opioid withdrawal, treatment facility admissions, drug overdose, and overdose-related deaths.
As a result of this epidemic (Figure 2), many states implemented prescription drug monitoring programs. These programs are intended to identify high-risk behaviors among patients and providers. The programs are also intended to facilitate referrals to substance abuse treatment programs and to and help healthcare providers created more effective prevention strategies.
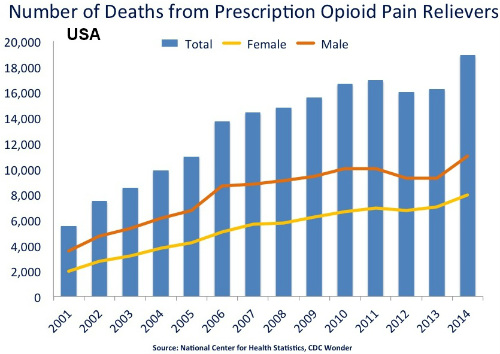
(Sources: Wikipedia/By National Institute on Drug Abuse.)
The Analysis
In the Health Affairs study, the authors “used an interrupted time-series design to examine the association of both implementation and characteristics of prescription drug monitoring programs with the rate of opioid-related overdose deaths.”
“We obtained data from multiple public sources (described below) for the period 1999–2013. Our analysis focused on the thirty-five states that implemented programs during the study period,” the authors explained.
They gathered data on the programs’ year of enactment of implementation. “A set of time-varying indicator variables was constructed for each state to capture when a prescription drug monitoring program statute passed and when the program was implemented. We also tested the interaction of the year a program was implemented with time, to determine if the association between opioid-related overdose deaths and implementation of a program changed over time. In addition, a set of indicators was created to identify program features, including the number of drug schedules monitored, the frequency of data updates, and whether or not registration or use was mandatory,” the authors added.
They examined bivariate and multivariate results to determine the primary outcome: whether implementation of a monitoring program resulted in a reduction in opioid-related overdose deaths. Linear regression models with state fixed effects modelling were used to account for unmeasured variation at the state level and for specific time-varying state-level factors. A secondary outcome was to determine if specific program characteristics were associated with greater changes in rates of opioid-related overdose deaths.
Results showed that, overall, the implementation of drug monitoring programs was associated with reductions in opioid prescribing, opioid-related overdoses, and opioid-related overdose deaths.
