- Use of gabapentin was linked to decreased opioid consumption following total knee arthroplasty (TKA).
- The use of gabapentin was also associated with a decreased incidence of pruritus in 6 randomized controlled (RCTs).
- The meta-analysis included 859 participants.
- No significant differences in Visual Analogue Scale (VAS) scores were detected between the gabapentin and placebo groups.
The addition of gabapentin reduced patient requirements for postoperative opioids and the incidence of pruritus following total knee arthroplasty (TKA; Figure 1), according to a meta-analysis of randomized controlled trials (RCTs). The results were published recently in the journal Medicine.
(Sources: By fpjacquot/Wikipedia/GNU Free/Creative Commons.)
The Analysis
In this case, the reviewers endeavored to determine the overall analgesic effect of gabapentin versus placebo following total knee arthroplasty (TKA). They conducted a search of the following electronic databases: PubMed, EMBASE, Ovid MEDLINE, ClinicalTrials.gov, and Cochrane Central Register of Controlled Trials from 1966 to June 2015. Randomized controlled trials were included in which gabapentin and placebo were compared for adjuvant analgesia following TKA. The meta-analysis was performed following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement.
The reviewers identified 6 trials including 859 participants (439 in the gabapentin group) which met the inclusion criteria. Gabapentin dosages ranged from 300 mg vs placebo to 1300 mg gabapentin vs. placebo. The primary endpoint was cumulative opioid consumption and the Visual Analogue Scale (VAS) scores at 12 hours, 24 hours, and 48 hours after the completion of surgery. Knee flexion degree and adverse effects associated with gabapentin were also compiled in order to evaluate safety (Figure 2).
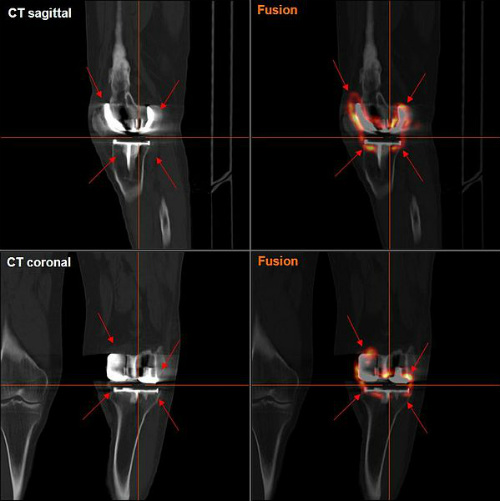
(Sources: By Hg6996/Wikimedia/Creative Commons CC BY 3.0.)
After testing for the heterogeneity and publication bias among studies, the reviewers aggregated data random-effects modeling. The reviewers found a significant decrease in morphine consumption at 12 hours: 4.69mg lower (95% CI: −7.18 to –2.21, P=0.0002); at 24 hours: -5.30mg lower (95% CI: −9.94 to –0.66, P=0.03); and at 48 hours: 17.80mg lower (95% CI: −31.95 to –3.64, P=0.01), respectively. Compared with the control group, the rate of pruritus was lower in the gabapentin group (RR 0.20, 95% CI 0.10 to 0.38, P=0.00). The most commonly reported adverse effect was nausea, which was reported in 5 of the 6 trials; 4 studies reported sedation as an adverse effect, and 3 studies reported dizziness. No significant differences were noted in VAS scores between the gabapentin and placebo groups. (Figure 3.)

in vivo measurements of forces and moments.
(Sources: Wikipedia/By Julius Wolff Institute, Team: Instrumented Implants, Charité - Universitätsmedizin Berlin/Creative Commons.)
“In summary, the administration of gabapentin was effective in decreasing postoperative narcotic consumption and the incidence of pruritus. There was a high risk of selection bias and a higher heterogeneity of knee flexion range in this analysis. More high-quality large randomized controlled trials with long follow-up period are necessary for proper comparisons of the efficacy and safety of gabapentin with placebo,” the authors concluded.
