- Purdue Pharma’s internal notes indicate the drug maker knew that OxyContin’s effectiveness falls well short of 12 hours in most patients.
- Many patients in Purdue trials were not getting 12 hours of pain relief.
- Purdue Pharma seems to have been aware of this fact since as early as 1996, according to the Los Angeles Times’ investigation.
- Purdue seems to have instructed physicians to prescribe increasing doses in patients who were not getting 12-hour analgesia.
An in-depth analysis of internal Purdue Pharma documents by the Los Angeles Times suggest that the drug maker was well aware that its drug, OxyContin (controlled-release oxycodone), did not provide the 12-hour analgesia that the company promoted.
The long duration of action so widely promoted by Purdue Pharma was among the strongest selling points for the drug which became the company’s No. 1 selling product, earning as much as $3 billion per year as early as 1996. OxyContin has maintained market leadership for 20 years and has also come to be seen as one of the root causes of the opioid epidemic that is currently ravaging American communities. Since 1999, more than 190,000 people have died in the U.S. from opioid-related overdoses, according to an article in Fortune as well as the U.S. NIH National Institute On Drug Abuse and the National Survey on Drug Use and Health (Figures 1 and 2). The 12-hour duration of action was the main selling point of OxyContin over generic oxycodone.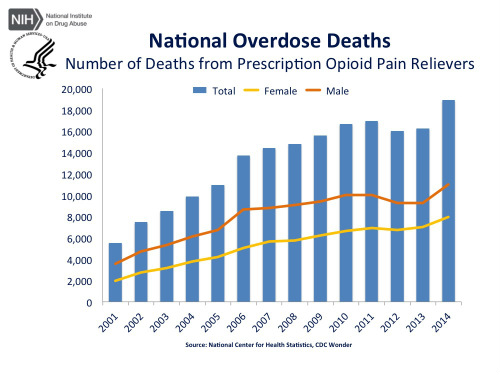
Over the years during which OxyContin has been on the market, the privately held Purdue Pharma has earned more than $35 billion from the drug, according to the LA Times report, as well as reports in Fortune and Forbes. According to Forbes Magazine these earnings made the Sackler family one of the richest families in the U.S. in 2015.
The 12-hour dosing schedule was essential to the market success of OxyContin and to Purdue Pharma’s enormous earnings. During the heady marketing days of OxyContin in the late 1990s, Purdue hired hundreds of well-respected pain physicians and thousands of sales reps to tell the story of OxyContin’s long duration.
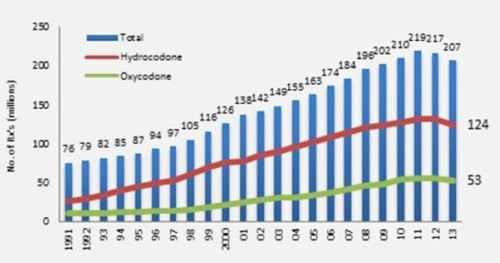
(Source: drugabuse.gov.)
However, many pain patients and the physicians who cared for them began to realize that OxyContin’s effectiveness often fell short of the touted 12 hours. Patients complained and asked for higher doses and physicians felt required to prescribe them. The movement to recognize pain as the 5th vital sign was being led by the American Pain Society, by thousands of pain physicians, and by the pharmaceutical companies who manufactured analgesics.
According to the LA Times article:
“When many doctors began prescribing OxyContin at shorter intervals in the late 1990s, Purdue executives mobilized hundreds of sales reps to “refocus” physicians on 12-hour dosing. Anything shorter “needs to be nipped in the bud. NOW!!” one manager wrote to her staff
Since then, “Over the last 20 years, more than 7 million Americans have abused OxyContin, according to the federal government’s National Survey on Drug Use and Health. The drug is widely blamed for setting off the nation’s prescription opioid epidemic, which has claimed more than 190,000 lives from overdoses involving OxyContin and other painkillers since 1999.
“The internal Purdue documents reviewed by The Times come from court cases and government investigations and include many records sealed by the courts. They span three decades, from the conception of OxyContin in the mid-1980s to 2011, and include emails, memos, meeting minutes and sales reports, as well as sworn testimony by executives, sales reps and other employees.”
According to the U.S. NIH National Institute On Drug Abuse:
“To illustrate this point, the total number of opioid pain relievers prescribed in the United States has skyrocketed in the past 25 years (Figure 1). The number of prescriptions for opioids (like hydrocodone and oxycodone products) have escalated from around 76 million in 1991 to nearly 207 million in 2013, with the United States their biggest consumer globally, accounting for almost 100% of the world total for hydrocodone (e.g., Vicodin) and 81% for oxycodone (e.g., Percocet).
“This greater availability of opioid (and other) prescribed drugs has been accompanied by alarming increases in the negative consequences related to their abuse. For example, the estimated number of emergency department visits involving nonmedical use of opioid analgesics increased from 144,600 in 2004 to 305,900 in 2008; treatment admissions for primary abuse of opiates other than heroin increased from 1% of all admissions in 1997 to 5% in 2007; and overdose deaths due to prescription opioid pain relievers have more than tripled in the past 20 years, escalating to 16,651 deaths in the United States in 2010. (Prescription drug deaths are a growing problem among women; Figure 3.)
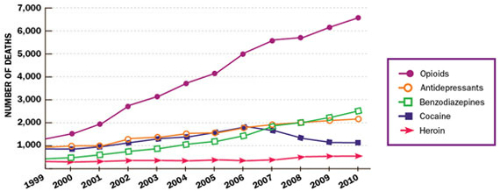
(Source: CDC.gov.)
We are not seeing the deadly effects of the movement to advance the use of opioid analgesia beyond use for terminal cancer pain and acute, postoperative pain. Today tens of thousands of Americans use these drugs. Many have become dependent and addicted. Many have died and many more lives have been lost. For every death that results from opioid overdose there is a family that may have exhausted its resources trying to help the addicted person. Many others have simply been shattered by the loss of a loved one. And, many of those that survived addiction to prescription opioids have turned to heroin due to its relatively low price and ease of availability (Figure 4).
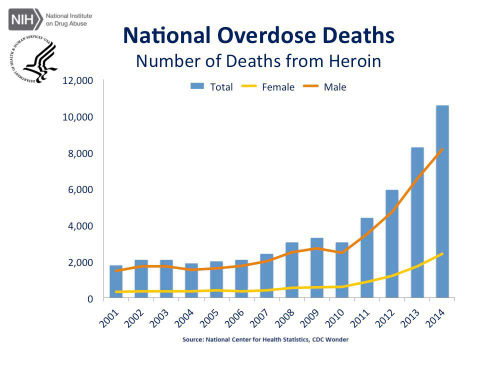
On a national level, the U.S. is spending hundreds of millions of dollars on the prevention and treatment of opioid addiction. Law enforcement agencies are significantly distracted by efforts to control the distribution of these drugs, and to both prevent the crimes that are associated with their use and to arrest and punish those who have committee such crimes. Insurance companies have similarly spent millions on the treatment of dependence and addiction.
The liberal attitude toward opioid prescription has begun to swing back again. Sadly, this will likely cause great suffering among many legitimate pain patients. Others will simply continue to turn to heroin.
