- Systematic review of randomized, controlled trials finds that mobile apps can benefit patients with chronic diseases.
- Review included 9 RCTs.
- Disease states included diabetes mellitus, cardiovascular diseases, and chronic lung diseases.
- Interventions ranged from automatic text messages to enhanced clinician contact.
Mobile device health (mHealth) apps can improve symptom management in chronic diseases, according a systematic review of randomized, controlled trials (RCTs). The study was published recently in the Journal of Medical Internet Research. The study included 9 RCTs but did identify the number of patients included in the trials. The U.S. Army and Navy have used telemedicine for more than 10 years (Figures 1 and 2).

to telecommunication between service members and mental healthcare counselors
which will give them more direct and immediate access to psychological therapy
in areas where counselors are sparse, July 30, 2012 at Joint Base Lewis-McChord, Wash.
(Sources: Wikipedia/U.S. Army.)
Self-management apps were defined as software designed for mobile phones and tablets with the aim of supporting self-management skills to manage key disease markers and symptoms.

(2006). Senior training specialist with Multi-Services Group International (MSGI),
Michael Bedwell, trains Sailors to use Battlefield Medical Information Systems Telemedicine (BMIST) equipped Personal Digital Assist's (PDA) aboard the Military Sealift Command (MSC) hospital ship USNS Mercy (T-AH 19).
(Sources: Wikipedia/U.S. Navy/Creative Commons.)
The reviewers conducted a Boolean search of the PubMed, Embase, and EBSCO databases for studies that assessed the effectiveness of apps in the management of chronic diseases and were published between 2005 and 2016. Due to the nature of the interventions, participants could not be blinded, so selection bias is a major confounder in this study.
“Studies were included from 4 geographic regions (Europe, n=3; Oceania, n=2; Asia, n=3; United States, n=1). All included studies were RCTs that assessed the effectiveness of interventions that involved mobile phone- or tablet-assisted self-management programs and either standard care (n=8) or offline self-management programs (n=1),” the authors wrote. Telemedicine systems are currently in use in many areas of the U.S. (Figure 3).
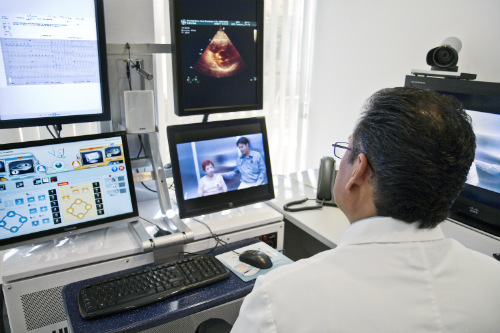
who is 640 km (400 mi) away in La Paz, Baja California.
(Sources: Wikipedia/IntelFreePress/Flickr/Creative Commons.)
The average age of participants ranged from 33.8 years to 72.1 years. One study reported that users aged >63 years were significantly more likely than younger patients to be substantial users of the app (P=0.045). Actual interventions included text messaging and phone conversations; 2 studies used automatic text messages generate by app data alone. Other studies included additional clinician input; 1 study standardized enhanced clinical input across the control and intervention groups. In 6 studies the level of clinician input and support for the intervention group was enhanced, the authors noted. “In these studies, the effect of using an app cannot be isolated, and the results cannot be interpreted in relation to increased clinician input or support and the use of an app,” they explained.
“Of the 5 studies that explored the impact of using an app only as the intervention tool on clinical outcomes, 3 studies demonstrated a significant change in symptom management and 2 did not. Only 1 study isolated the contribution of the app intervention where clinical care was standardized for the intervention and control group. The study did not report a significant change in asthma symptom control, with symptom control improving marginally in both groups,” the authors explained.
Conclusions
“The evidence indicates the potential of apps in improving symptom management through self-management interventions. The use of apps in mHealth has the potential to improve health outcomes among those living with chronic diseases through enhanced symptom control. Further innovation, optimization, and rigorous research around the potential of apps in mHealth technology will move the field toward the reality of improved health care delivery and outcomes,” the reviewers concluded.
