- Patients are living longer with cancer pain.
- There is an urgent need for clinicians to provide analgesia without tolerance, dependence, or somnolence.
- Evidence supports the use of numerous non-opioid analgesics, as well as devices and techniques are available.
- Cancer-related pain can be effectively relieved or mitigated through the combination of a number of strategies.
Pain is a frequent sign of many cancers. The pain can be a result of tumor directly stimulating pain receptors (Figure 1), or by tumors within the nerves themselves. Tumors in bone are known to be particularly painful. The pain can be localized, or it can be distant and distributed as a result of metastatic disease.
Iatrogenic pain and pain syndromes are common in cancer patients. Uncontrolled pain in lung cancer is linked to patient distress, depression, and fatigue. Patients regularly report pain as the most disliked side effect of cancer and its treatment. It has a profoundly negative effect on quality of life.
The good news is that cancer-related pain can be effectively relieved or mitigated through the combination of a number of strategies. Depending on the source of the pain, opioids, nonopioid analgesics, anti-seizure drugs, psychiatric medications, interventional techniques such as analgesic pain pumps, or transcutaneous electrical nerve stimulation (TENS; Figure 2), yoga, tai chi, reiki, meditation, exercise, acupuncture, and hypnotism have all been shown to benefit patients in chronic pain. The proper combination of these approaches can help the physician and the patient achieve significant, enduring pain relief.

Pain management in lung and other forms of cancer is frequently guided in part by the philosophy behind theWorld Health Organization's (WHO) analgesic ladder for cancer pain relief (Figure 3). Treatment begins with nonsteroidal anti-inflammatory drugs and acetaminophen. If the pain remains uncontrolled, weak opioids are started. The third step in the treatment of the refractory pain of advanced disease is to prescribe strong opioids.
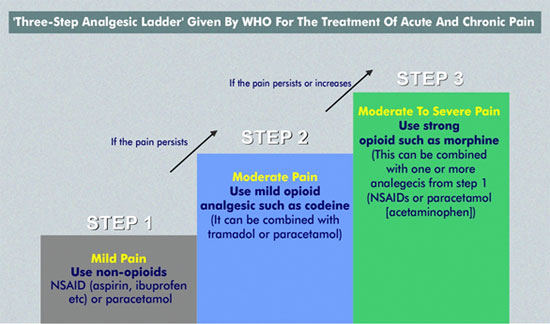
The clinical truth of chronic pain management is more complicated than the WHO analgesic ladder would suggest. Adjuvants to pain control, such as selective serotonin reuptake inhibitors (SSRIs), tricyclic antidepressants, serotonin-norepinephrine reuptake inhibitors (SNRIs), anticonvulsants, and alpha2-adrenergic agonists, are also used.
Other non-opioid options for treating cancer pain include N-methyl-d-aspartate (NMDA) antagonists, which can be especially helpful for patients who have developed a tolerance for opioids. Pain related to increasing intracranial pressure, neuropathy, and lymphedema may be relieved by adding corticosteroids, with the risk for side effects taken into account. Topical analgesics are helpful for localized pain and are associated with fewer systemic side effects.
When considering more invasive procedures for pain relief such as implanted analgesic pumps and nerve stimulators, or nerve ablation, the oncologist and the patient can weigh the risks and benefits. Procedural forms of cancer relief may allow another option for patients who have side effects from opioids. Pain management may take the form of nerve blocks, continuous analgesic infusions, dorsal sensory root (Figure 1) ablation, interpleural analgesia, and epidural and spinal analgesia.
Locally advanced and metastatic NSCLC leads not only to pain but also to weight loss, depression, dyspnea, and cough. A palliative care team may be able to offer measures associated with longer survival, reduced symptoms, and improved quality of life. Thoracic external beam radiation treats pain and can also relieve cough, hemoptysis, and dyspnea. External beam radiation, laser therapy, brachytherapy, and photodynamic therapy can alleviate central airway obstruction and associated symptoms. A combination of radiation, ablation, and pharmacologic treatment may be required for symptoms secondary to lung metastasis.
Further Reading
- Aspirin and nonsteroidal anti-inflammatory drugs can prevent cutaneous squamous cell carcinoma: a systematic review and meta-analysis. Muranushi C, Olsen CM, Pandeya N, Green AC. J Invest Dermatol. 2015;135(4):975-83.
- Prophylactic use of aspirin: systematic review of harms and approaches to mitigation in the general population. Thorat MA, Cuzick J. Eur J Epidemiol. 2015;30(1):5-18.
- [Opioids in chronic noncancer pain-are opioids superior to nonopioid analgesics? A systematic review and meta-analysis of efficacy, tolerability and safety in randomized head-to-head comparisons of opioids versus nonopioid analgesics of at least four week's duration]. Welsch P, Sommer C, Schiltenwolf M, Häuser W. Schmerz. 2015;29(1):85-95.
- American Cancer Society. Side effects of targeted cancer therapy drugs. Revised December 11, 2014. Accessed September 20, 2015.
- Bath C. Lung cancer expert offers recommendations for treating toxicities associated with targeted therapies. The ASCO Post. December 15, 2014. Accessed September 20, 2015.
- Center for Drug Evaluation and Research (CDER) and Center for Biologics Evaluation and Research (CBER), U.S. Food and Drug Administration (FDA). The voice of the patient: a series of reports from the U.S. Food and Drug Administration’s (FDA’s) patient-focused drug development initiative. Lung cancer. Published December 2013. Accessed September 20, 2015.
- Davies M. New modalities of cancer treatment for NSCLC: focus on immunotherapy. Cancer Manag Res. 2014;6:63-75.
- Elice F, Rodeghiero F. Side effects of anti-angiogenic drugs. Thromb Res. 2012;129 Suppl 1:S50-S53.
- Reck M, Heigener DF, Mok T, Soria JC, Rabe KF. Management of non-small-cell lung cancer: recent developments. Lancet. 2013;382(9893):709-719.
- Silva S, Danson S. Targeted therapy and new anticancer drugs in advanced disease. Thorac Surg Clin. 2013;23(3):411-419.
- Simmons CP, Macleod N, Laird BJ. Clinical management of pain in advanced lung cancer. Clin Med Insights Oncol. 2012;6:331-346.
- Simone CB, Jones JA. Palliative care for patients with locally advanced and metastatic non-small cell lung cancer. Ann Palliat Med. 2013;2(4):178-188.
- Sundar R, Soong R, Cho BC, Brahmer JR, Soo RA. Immunotherapy in the treatment of non-small cell lung cancer. Lung Cancer. 2014;85(2):101-109.
