- Pain specialists are increasingly suggesting that opioid analgesia be reserved for patients who do not respond to all other available pain therapies.
- An increasingly wide variety of drug types are being used to effectively treat patients in pain.
- Always request a pregnancy test in any woman of childbearing years before prescribing an opioid analgesic.
Schaumburg, IL—Many young women do not know they are pregnant for several weeks or months after conception. For this reason, the national Centers for Disease Control and Prevention (CDC) recently raised an alarm about high rates of opioid prescriptions among women of childbearing age and the potential for birth defects.1 (See Figure.)
But how should primary care physicians, obstetricians, and other physicians help their female patients deal with pain, especially back pain in young women?
- Request a pregnancy test. Obviously, you will want to know as early as possible whether your patient is pregnant. This will influence the remainder of her treatment.
- Recommend yoga first. According to research published in the Journal of Evidence-Based Complementary & Alternative Medicine, 12 weeks of yoga significantly relieved back pain in women. Women with back pain who did not do yoga reported worsening pain over the same period.2 For pregnant women especially, yoga provides a safe alternative to opioids, which “early in pregnancy can cause birth defects and serious problems for the infant and the mother,” said CDC Director Tom Frieden, MD, MPH.
- If surgery is necessary, shy away from general anesthesia. Women report less pain and less nausea, use less morphine and leave the hospital faster after surgery when they receive regional analgesia plus I.V. anesthesia, according to a study in Anesthesiology.3
- Consider complementary and alternative therapies for other kinds of pain. Obstetricians may want to recommend that their patients build a labor playlist, as listening to music during labor reduces pain and anxiety during childbirth and improves maternal blood flow and infant heart rates. Women who rocked out also need less pain medication after birth.4 Ob-gyns may want to stock some essential oils, as well. A study in the Journal of Obstetrics and Gynaecology found that girls and women with cramps who massage their abdomens with rose oil experienced much less pain.5
Consider non-traditional analgesics. Anticonvulsants and various types of antidepressant drugs have been shown to be effective for patients with various types of pain. When treating pain patients, always consider consulting with a specialist. There are many benefits for both patients and providers to reserving opioid therapy as a last-resort clinical decision. Pain specialists are increasingly suggesting that opioid analgesia be reserved for patients who do not respond to all other available therapies.
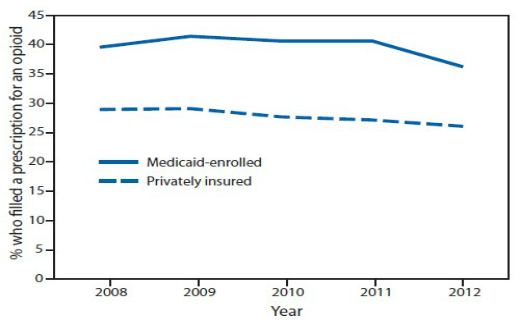
Source: Truven Health Marketscan Commercial Claims and Encounters and Medicaid Data.
1. Ailes EC, Dawson AL, Lind JN, Gilboa SM, Frey MT, Broussard CS, Honein MA. Division of Birth Defects and Developmental Disabilities, National Center on Birth Defects and Developmental Disabilities, CDC. Opioid prescription claims among women of reproductive age — United States, 2008–2012. MMWR Morb Mortal Wkly Rep. 2015;64:37-41.
2 Lee M, Moon W, Kim J. Effect of Yoga on Pain, Brain-derived Neurotrophic Factor, and Serotonin in Premenopausal Women with Chronic Low Back Pain. Evidence-Based Complementary and Alternative Medicine. Vol. 2014, Article ID 203173, 7 pages.
3. Abdallah FW, Morgan PJ, Cil T, McNaught A, Escallon JM, Semple JL, Wu W, Chan VW. Ultrasound-guided Multilevel Paravertebral Blocks and Total Intravenous Anesthesia Improve the Quality of Recovery after Ambulatory Breast Tumor Resection. Anesthesiology, 2014;120(3):703
4. Simalvi S, Gumus I, Kaygusuz I, Yildirim M, Usluogullari B, Kfali H. Effect of music on labor pain relief, anxiety level and postpartum analgesic requirement: A randomized controlled clinical trial. Gynecologic and Obstetric Investigation. 2014;78(4):213-280.
5. Sadeghi Aval Shahr H, Saadat M, Kheirkhah M, Saadat E. The effect of self-aromatherapy massage of the abdomen on the primary dysmenorrhoea. J Obstet Gynaecol. 2014;25:1-4.
