- Having social connections improves peoples’ odds of survival by 50% on average.
- Living alone increased the likelihood of mortality the most, 32%, while social isolation raised the risk by 29% and loneliness by 26%.
- Simply living with someone else increased survival by nearly 20%.
- Extensive social integration nearly doubled the odds of survival.
Telling a Patient to Spend Time with Friends is Medical Advice
Of course you advise an alcoholic patient to seek help to stop drinking, and you would offer a smoker ways to stop smoking. Similarly, the time has come to ask patients about their social lives, and to offer advice to help them become more social, if necessary. Socializing is likely the most inexpensive way to reduce mortality related to loneliness among adults. (See Figure.)
You can find our brief literature review on the relationship between loneliness, social isolation, and physical health here.
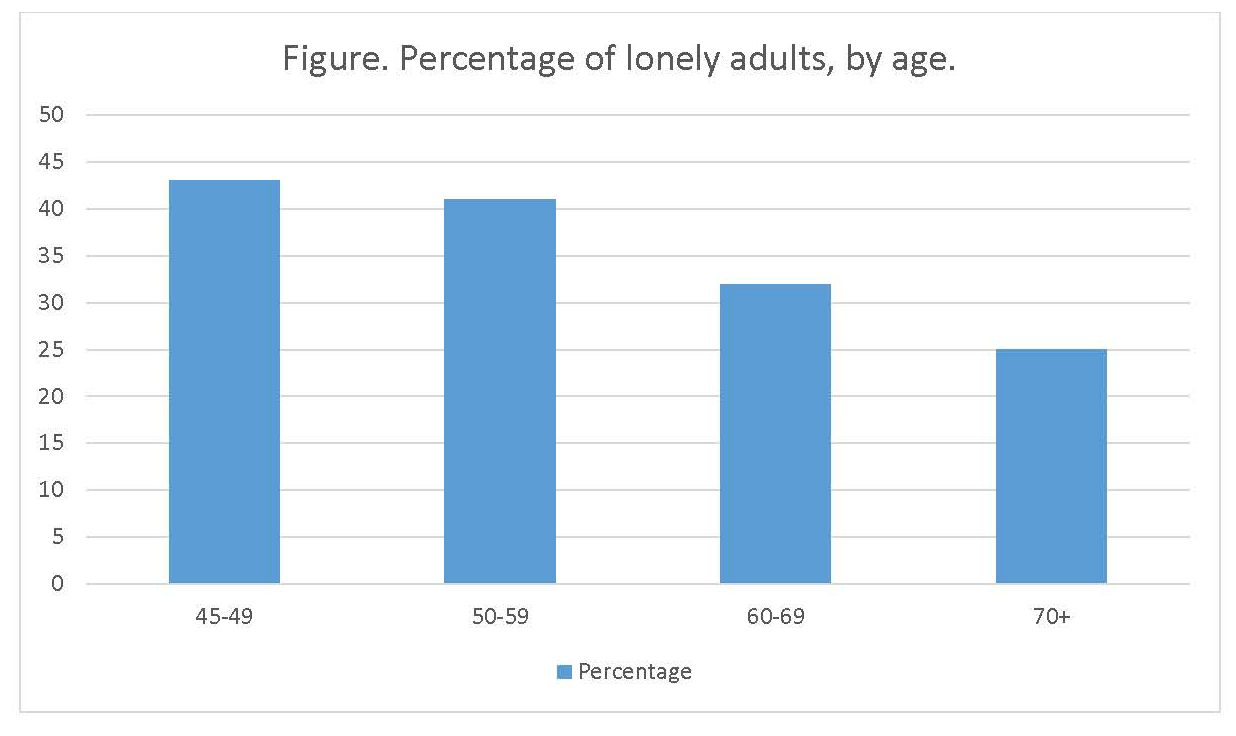 Based on research from Pew Research Center, 2009 and AARP, 2011.
Based on research from Pew Research Center, 2009 and AARP, 2011.
“We need to start taking our social relationship more seriously,” said lead author Julianne Holt-Lunstad, PhD, Professor of Psychology at Brigham Young University.
You might want to start asking your patients this pair of screening questions: “Are you lonely?” and “Are you socially active?”
If your patients indicate that they experience social isolation, you may want to prescribe a little more interaction with others. This can come through taking up hobbies that bring them into contact with others, saying hello to their neighbors, becoming regulars at a coffee shop or gym, volunteering, join a walking club or book club, talking more often with friends and family on the phone and in person, or connecting through social media, or through Skype.
All those steps build relationships and, in turn, appear to protect physical and psychological health.
“When someone is connected to a group and feels responsibility for other people, that sense of purpose and meaning translates to taking better care of themselves and taking fewer risks,” said Dr. Holt-Lunstad.
Good Medicine
Regardless of your medical specialty, the answers to those questions will likely influence how your patients respond to treatment -- and their overall health. Both the subjective experience of loneliness and the objective experience of social isolation significantly increase the risk of a host of negative medical outcomes from pain and depression to more severe breast cancer symptoms to mortality, according to articles in Psychoneuroendocrinology 2013;38:1310–1317 and Breast Cancer and Treatment (2013:139:515-527).
Feeling lonely, but not social isolation, was predictive of increased risk of dementia, according to an article in the Journal of Neurology, Neurosurgery, and Psychiatry (2014;85:135-42). People who felt lonely also experienced difficulty sleeping, according to a study of 95 South Dakotans published in Sleep (2011;34:1519-26).
Both Being Alone and Feeling Lonely are Deadly
According to the results of a systematic review published in JAMA (2013;309:71-82). Living alone increased the likelihood of mortality the most, 32%, while social isolation raised the risk by 29% and loneliness by 26%. The negative influence of social isolation persisted across gender, length of follow-up and world geography, but were more predictive of death in those less than 65 years of age. For comparison, a body mass index of more than 35 (grade 2 or higher obesity) is associated with a 29% increase in all-cause mortality.
On the flip side, having social connections improves one's odds of survival by 50% on average, according a meta-analysis published in PLOS Medicine (2010;7:e1000316. PMID: 20668659) by the same researchers. Simply living with someone else increased survival by nearly 20%, while more extensive social integration nearly doubled the odds of survival. That study found that low social interaction reduced longevity to the same degree as smoking 15 cigarettes per day or long-term alcohol abuse.
