- At around $70 per kit, this may be the most cost-effective life-saving intervention available to physicians.
- The opioid epidemic is arguably the most significant current public health emergency in the U.S.
- Depending on geography, the cost of an overdose survival is ~$10,000.
- The average cost of an overdose-related death at the MetroHealth System in Cleveland, Ohio, is approximately $3000.
- Naloxone kit distribution programs can be run at a cost of <$1000/life saved.
Naloxone Distribution Programs
Naloxone distribution programs have become increasingly common throughout the U.S where support is surprisingly strong and widespread. Where needle exchange programs have not been able to take hold, the distribution of naloxone kits has bipartisan support, even in relatively conservative states such as Ohio.
“This is the largest public health crisis that we have right now,” Joan Papp, MD, told MDalert.com. Dr. Papp is Medical Director for Project DAWN, a naloxone distribution program run by the MetroHealth System in Cleveland, Ohio.
“I think that naloxone programs are drastically under-utilized,” she said. “These programs are one of the best ways that we have to drastically impact mortality. These programs can be implemented in a variety of settings. I think it is so important that all healthcare providers are aware that this is something they can prescribe today. This should be a part of everyday prescribing,” depending on your practice.
MetroHealth operates 3 walk-in clinics in Cuyahoga County, Ohio, and another through the Cleveland Free Clinic, an independent care provider.
See our brief literature review on naloxone distribution programs here.
According to one of the few studies of the cost-efficacy of naloxone programs, Coffin and Sullivan found that “Naloxone distribution to heroin users is likely to reduce overdose deaths and is cost-effective, even under markedly conservative assumptions,” according to a report in the Annals of Internal Medicine (Ann Intern Med. 2013;1581:1-9).
These findings were the result of a mathematical model study. The researchers used “Integrated Markov and decision analytic model using deterministic and probabilistic analyses and incorporating recurrent overdoses and a secondary analysis assuming heroin users are a net cost to society.”
Project DAWN
“I have been surprised by how much support we’ve had here,” Dr. Papp, speaking of the state of Ohio. “We have gotten support on both sides of the aisle. We had bipartisan sponsorship for our first bill and a Republican sponsor for the second [current] bill. Both of our bills have passed unanimously in both [state] houses in 2 decisions,” Dr. Papp noted. “I have been amazed by how much support we have had for naloxone in Ohio.”
Project DAWN currently runs a budget of about $200,000. However, in the first year, beginning in March 2013, the annual budget was about $90,000 and remained at this level for the first 18 months of the program. Project DAWN serves all of Cuyahoga County (pop. 1.2 million) and most of metropolitan Cleveland, Ohio (pop. 2.1 million).
“MetroHealth and Project DAWN do not turn individuals away based on county of residency. In fact, we see patients from all over Ohio who come to access our services,” explained Emily Metz, in an interview with MDalert.com. Ms. Metz is the Project DAWN Program Coordinator.
Since it began in March, 2013, Project DAWN has given out more than 2000 naloxone kits. Of those, more than 220 have been reported to have been used in reversals. The calculation using the most conservative possible numbers yields a cost per life saved of about $700.
On the other hand, the cost per patient hospitalized at MetroHealth for an opioid overdose is at least $10,000. The lethal overdose costs the hospital nearly $3000. Since the program began, the hospital has saved more than $320,000 attributable to Project DAWN alone, according to Ms. Metz.
For every reversal voluntarily reported to Project DAWN, between 10 and 11 kits must be distributed. The number of times that Project DAWN kits are used is very likely under-reported, because the Project DAWN staff must rely on individuals to come back to the program to report a rescue.
It is worth noting that the number needed to treat (NNT) for this intervention is close to the ideal of 1. In very nearly every case, a person who would otherwise die is simply retrieved from the edge and brought back to life.
North Carolina Harm Reduction Coalition
“Reporting successful overdose reversals is one of the biggest challenges that naloxone distribution programs face,” Tessie Castillo blogged in The Huffington Post. Ms. Castillo is the Advocacy and Communications Coordinator for the North Carolina Harm Reduction Coalition (NCHRC).
Inaccurate reporting underestimates the number of lives saved by these programs. “In many cases, an outreach worker will distribute a naloxone kits to a person at risk for opiate drug overdose, and then never see or hear from that person again. Most drug users, already reluctant to admit to activity due to social stigma, will use the kit and never tell anyone unless they have an established, trusting relationship with the person or organization who gave them the kit. So how can you tell if your program is actually working?”
Inaccurate reporting aside, the numbers are still excellent for naloxone distribution programs. The NCHRC has distributed more than 10,500 kits, according to the report in The Huffington Post. Of these, 586 have been reported to have been used in overdose reversals. The kits cost about $70 each meaning that even once salaries are paid and space is rented, these kits cost less than $2000 per life saved.
This is simply an astounding number. Any physician who wants to save lives and cut costs should start to advocate for the distribution of naloxone kits.
Code?
Statistical inaccuracies are the product of multiple social pressures but they are also generated within the hospital. “There is not very good consistency” in coding, noted Dr. Papp. “Sometimes it just gets coded as ‘overdose.’ Sometimes it gets coded as a psych case” when the signs are more likely related to opioid intoxication or withdrawal.
“We also have patients who try to convince us that they have a disorder for which opioids would be appropriate, such as pain or withdrawal. This is a real challenge.” It can be hard to distinguish these 2 groups, and the cost of making the wrong call can mean that the patient suffers unnecessarily or that his life is at risk again from overdose. The clinical and interpersonal challenges of this relationship are explored in a recent blog post by a physician, Danielle Ofri, MD, in The New York Times.
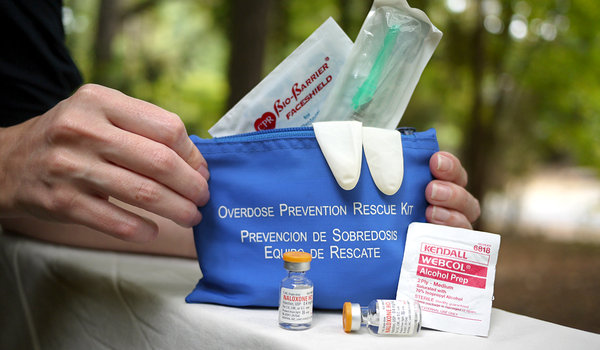
Naloxone (brand names include Narcan and Evzio) kits have become increasingly widely carried by police officers and Emergency Medical Service (EMS) professionals as the recent epidemic of opioid related deaths and hospitalizations has grown. Many healthcare providers are advocating for the still wider availability of these kits.
Naloxone is a competitive enkephalin antagonist. “Naloxone temporarily blocks the effects of opioids for about 30-90 minutes,” Ms. Metz explained. “Depending on the opioid and the physiology of the person who has ingested the drug or drugs, among other factors, the overdose victim could fall back into an opioid overdose once [the naloxone] has worn off. Naloxone is short-acting whereas many opioids are long acting.”
Whether the patient is opioid naïve or has experience with the drugs, it is unlikely that withdrawal will occur as a result of naloxone administration.
You Can Prescribe a Naloxone Kit
It is essential for all physicians to know that they can prescribe naloxone. In no state in the U.S. is the prescription of naloxone even highly regulated. Any physician can prescribe naloxone to a patient who is at risk of opioid abuse and overdose and any bystander can administer naloxone.
