- Postoperative myocardial infarction (MI) is the 3rd leading cause of death in the U.S.
Intraoperative hypotension, arterial occlusion and other phenomena appear to be part of the multifactorial causes.
Intraoperative clonidine is not protective against this phenomenon.
- Perioperative aspirin use was not related to intraoperative or postoperative MI.
Published in collaboration with our partners at Anesthesiology News.
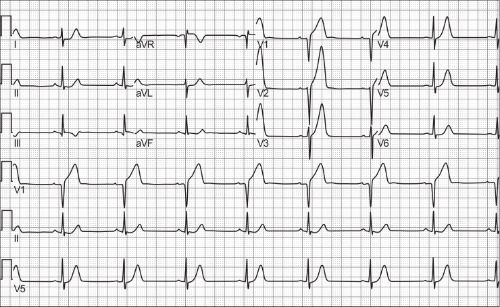
Something is killing thousands of patients in the 30 days following noncardiac surgery. While the cause remains elusive, members of the Outcomes Research Consortium (ORC) are looking for answers. “What we do know is that among patients aged ≥45 years, 10% will suffer a myocardial infarction (MI) (Figure 1) in the 30 days following surgery,” according to Daniel Sessler, MD.
The majority of these MIs are silent and not detected intraoperatively. Nonetheless, patients who suffer them exhibit the same physiologic responses and biomarkers as if the heart attack had been detectable. The ORC have examined intraoperative troponin and clonidine, as well as perioperative aspirin in an effort to find the cause.
Two clinician researchers, Daniel Sessler, MD, and Phillip Devereaux, MD, have led the research that endeavors to find the cause of this deadly phenomenon. Dr. Sessler speculated on the cause in an interview with MDalert.com. “Intraoperative hypotension appears to be the cause,” he said. “When mean arterial pressure [MAP] drops below a threshold of about 66mmHg the rate of MI starts to increase. When MAP reaches 55mmHg for one minute or more the risk of death increases significantly. The longer MAP hypotension is maintained, the higher the risk. This phenomenon is a leading cause of death.”
“Our theory,” Dr. Sessler continued, “is that a supply/demand mismatch is causing the myocardial infarction. An already narrowed artery coupled with operative hypotension seems to be responsible,” he explained.
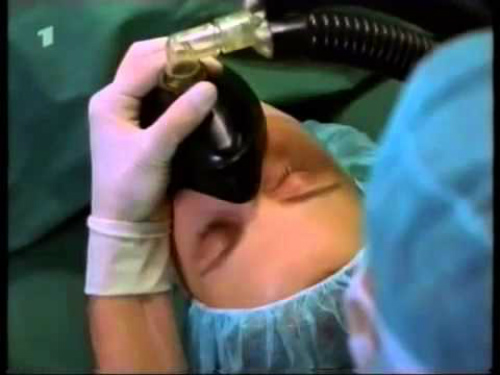
Dr. Devereaux reiterated this theory that added that “the cause is multifactorial. There is a supply/demand mismatch during surgery. Blood loss and narrowed cardiac vasculature coupled with intraoperative hypotension and other causes are likely at fault,” he explained. General anesthesia (Figure 2) as well as bleeding and drugs administered during surgery can cause drops in MAP.
Dr. Devereaux was the primary investigator in the VISION, POISE-1, and POISE-2 trials that identified the phenomenon and examined the effects of perioperative aspirin and intraoperative clonidine on MI and survival following noncardiac surgery. He is University Scholar and Professor in the Departments of Clinical Epidemiology, Biostatistics, and Cardiology at McMaster University Health Sciences Centre in Hamilton, Ontario, Canada.
Research
“In a series of huge trials,” Dr. Sessler explained. “The groups have shown that perioperative myocardial injury is common, clinically silent, deadly, and hard to prevent. Hypotension, though, appears to contribute and several Consortium studies show strong associations between hypotension and postoperative mortality,” he explained. These findings are just the most recent example of Dr. Sessler, Dr. Kurz, and their collaborators exposing phenomena that are exceedingly important to patients and clinicians. The researchers continue to do this through the conduct of meticulous scientific research.
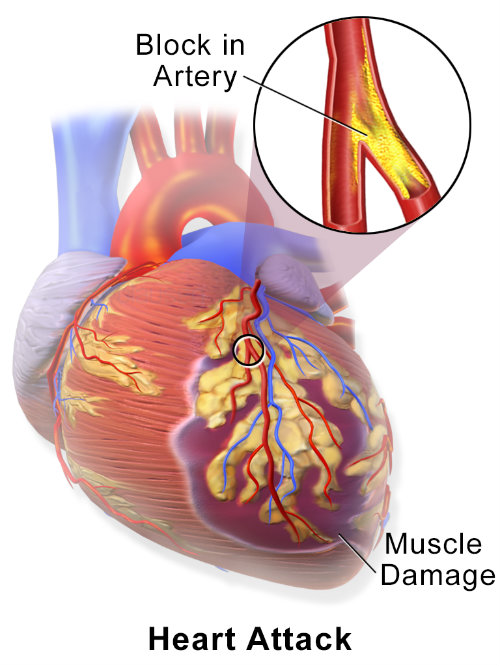
“Although lower mean arterial pressure is strongly associated with mortality, lower intraoperative blood pressure variability per se is only mildly associated with postoperative mortality after noncardiac surgery,” concluded Edward Masha, PhD, et al in in a review of data on 104,401 patients published in Anesthesiology (2015; 123:79-91). Myocardial infarction (Figure 3) is the cause of these postop deaths. The data were extracted from noncardiac surgery cases performed at Cleveland Clinic.
“In confounder-adjusted models, the authors evaluated the associations between 30-day mortality and both time-weighted average intraoperative mean arterial pressure (TWA-MAP) and measures of intraoperative MAP variability—including generalized average real variability of MAP (ARV-MAP) and SD of MAP (SD-MAP),” according to the article abstract.
Mean±SD TWA-MAP was 84±10 mmHg, and ARV-MAP was 2.5±1.3 mmHg/min, in these cases. TWA-MAP was strongly related to 30-day mortality, which more than tripled as TWA-MAP decreased from 80 to 50 mmHg. ARV-MAP was only marginally related to 30-day mortality (P=0.033) after adjusting for TWA-MAP. Odds of 30-day mortality decreased as five-level categorized ARV-MAP increased (0.92; 0.87 to 0.99 for one category increase; P=0.015). Cumulative duration of MAP <50, 55, 60, 70, and 80 mmHg was associated with increased odds of 30-day mortality (all P<0.001), the authors reported
The POISE-1 collaborators conducted a 2-by-2 factorial trial (n=10,100) to examine the effects of perioperative aspirin use on 30-day mortality in these patients. Patients were stratified according to whether they had been taking aspiring before the study began; the initiation stratum (n=5628) and the continuation stratum (n=4382). Following the first stratification, patients started taking aspirin 200mg/d or placebo before surgery and continued aspirin 100mg/d for 30 days in the initiation stratum and ad for 7 days in the continuation stratum following surgery. The article was published in The New England Journal of Medicine (2014;370:1494-1503).
“The primary outcome occurred in 351 of 4998 patients (7.0%) in the aspirin group and in 355 of 5012 patients (7.1%) in the placebo group (hazard ratio in the aspirin group, 0.99; 95% confidence interval [CI], 0.86 to 1.15; P = 0.92),” the authors wrote. “Administration of aspirin before surgery and throughout the early postsurgical period had no significant effect on the rate of a composite of death or nonfatal myocardial infarction but increased the risk of major bleeding,” they concluded.
The POISE-2 trial investigated the relationship between the use of low-dose clonidine and risk of death or nonfatal MI within the 30 postoperative days. This trial was also a 2-by-2 factorial trial that included 10,010 patients and was published in New England Journal of Medicine (2014;370:1504-13).
“Clonidine, as compared with placebo, did not reduce the number of primary-outcome events (367 and 339, respectively; hazard ratio with clonidine, 1.08; 95% confidence interval [CI], 0.93 to 1.26; P=0.29). Myocardial infarction occurred in 329 patients (6.6%) assigned to clonidine and in 295 patients (5.9%) assigned to placebo (hazard ratio, 1.11; 95% CI, 0.95 to 1.30; P=0.18),” the authors noted.
“Administration of low-dose clonidine in patients undergoing noncardiac surgery did not reduce the rate of the composite outcome of death or nonfatal myocardial infarction; it did, however, increase the risk of clinically important hypotension and nonfatal cardiac arrest,” they concluded.
The Vascular Events In Noncardiac Surgery Patients Cohort Evaluation (VISION) Study Investigators, conducted a prospective international cohorts trial that enrolled patients from 2006 to 2011. All patients (n=15,133) were aged ≥45 years and required at least 1 overnight hospital stay. The study was published in the New England Journal of Medicine (2012;307[21]:2295-304).
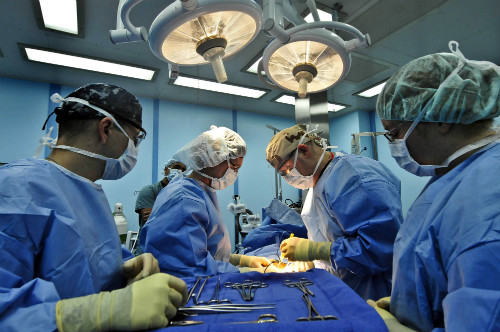
This study was intended to determine the relationship between the peak fourth-generation troponin T (TnT) measurement in the first 3 days following noncardiac surgery (Figure 4) and 30-day mortality. “Patients' TnT levels were measured 6 to 12 hours after surgery and on days 1, 2, and 3 after surgery. We undertook Cox regression analysis in which the dependent variable was mortality until 30 days after surgery, and the independent variables included 24 preoperative variables,” the authors wrote.
They concluded that “Among patients undergoing noncardiac surgery, the peak postoperative TnT measurement during the first 3 days after surgery was significantly associated with 30-day mortality.”
“Hypotension is likely the bad actor in this picture,” Dr. Sessler explained. “The threshold for injury seems to be an intraoperative mean arterial pressure (MAP) of ≤66mmHg,” He explained. “Maintaining a patient’s MAP at ≤55mmHg for 1 minute or more significantly increases the risk of death. The longer hypotension is maintained, the higher the risk of death in the 30-day postoperative period.”
period following noncardiac surgery.
The Outcomes Research Consortium
These trials were conducted within the ORC which was founded by Dr. Sessler in 1990 at the University of California, San Francisco (USCF). The Consortium’s administrative center moved from UCSF to the University of Louisville in 2000, and in 2005 it moved to the Anesthesiology Institute at Cleveland Clinic where it remains. In 1995, Andrea Kurz, MD, was appointed as the group’s Associate Director. Today, Dr. Sessler is the Michael Cudahey Professor and Chair of the Department of Outcomes Research at Cleveland Clinic, Cleveland, Ohio. Dr. Kurz is Chair of the Department of General Anesthesiology at Cleveland Clinic.
Today, the ORC includes more than 120 investigators in 10 countries. The ORC currently coordinates more than a 100 studies, including a dozen large, multi-center outcome trials. Collaboration is one of the essential aspects of Outcomes Research. Independent researchers collaborate within the ORC and the ORC itself routinely collaborates with two other large anesthesia trial groups, the Population Health Research Institute, and the Australian and New Zealand College of Anaesthetists Trials Network.
The Consortium’s has published more than 950 peer-reviewed articles in the most important medical journals in the world. About 200 of these papers have been published in Anesthesiology, approximately another 200 have been published in Anesthesia & Analgesia. Many others have appeared in the New England Journal of Medicine, the Journal of the American Medical Association, and The Lancet. ORC publications have been cited about 30,000 times, according to Dr. Sessler.
